
From Ambiguity to Action: How Claims Status AI Transforms Reimbursement Workflows
Tackling a Significant RCM Bottleneck
Revenue cycle teams know the frustration of vague payor responses, particularly the A-321 claim status code. This code is commonly used to signal “missing or invalid information,” yet it provides no further detail, making it one of the most problematic messages teams must interpret. Lacking actionable clarity, teams are left to manually review claims and reassign them to specific codes, which slows payment cycles and adds cost.
XiFin has taken direct aim at this challenge by embedding Claims Status AI into the Empower RCM platform. Using Natural Language Processing (NLP), the solution automatically translates ambiguous A-321 responses into clear, actionable reason codes, eliminating the need for manual intervention, accelerating resolution, and improving cash flow.
How Claims Status AI Works
Instead of manually assigning A-321 messages to actionable codes, the NLP model scans unstructured payor notes attached to these claims and identifies the underlying issue. It then updates claim status with high-confidence predictions, such as:
- Invalid diagnosis code
- Subscriber ID mismatch
- Procedure code is not a covered service
- Member is not on file
By transforming an ambiguous claim status into a specific, structured, and actionable one, the model not only reduces manual review but also streamlines workflows through auto-routing and prioritization.
Key Benefits for Revenue Cycle Teams
AI for A-321 claim status delivers measurable improvements across four key dimensions:
- Actionable Intelligence: Vague payor responses become clear next steps.
- Faster Payment Velocity: At-risk claims are identified early and resolved sooner, accelerating cash flow.
- Denial Prevention and Rework Reduction: Root causes are surfaced upfront, reducing costly resubmissions.
- Smarter Workflows: Claims are auto-assigned to minimize administrative burden and reduce the cost to collect.
The model also improves over time, learning from historical patterns to increase accuracy and forecast reimbursement velocity with greater confidence.
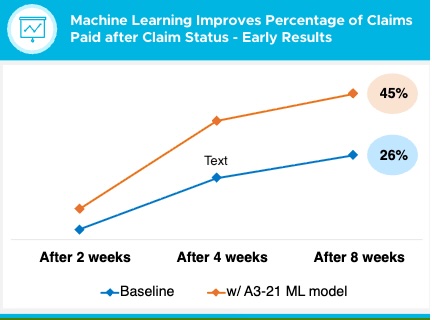
Tangible Results: One XiFin Customer Achieved a 73% Improvement in Reimbursement Velocity in Just 8 Weeks
The impact is already clear. Within eight weeks of implementation, one national diagnostic provider saw:
- Thousands of claims automatically re-coded from “A-321” to specific issue categories.
- 45% of AI-processed claims paid within the period, compared to only 26% with traditional manual handling—a 73% improvement in reimbursement velocity.
- Significant reduction in manual reviews, freeing staff to focus on higher-value work.
This acceleration in reimbursement translates directly to better cash flow and reduced days in accounts receivable.
Why It Matters for RCM Leaders
For healthcare providers, the difference between “pending” and “paid” often comes down to clarity. By transforming vague payor responses into precise next steps, Claims Status AI eliminates a persistent revenue cycle management bottleneck—one that contributes significantly to downstream denials, as detailed in XiFin’s 2025 Payor Denial Impact Report.
The takeaway: AI doesn’t just promise efficiency—it delivers it. When embedded directly into workflows, it drives more payments, faster denial management, and smarter resource allocation.
Looking Ahead
XiFin is committed to continuing to innovate, expand, and deliver various types of AI, including agentic, within the XiFin Empower portfolio. Subscribe to the XiFin Blog today to be the first to receive notifications about new AI-powered documentation and correspondence handling and appeals preparation and management. Claims Status AI is just one more milestone in our mission to help providers achieve greater financial results without adding complexity or requiring additional investment.
Connect with XiFin to learn more about Claims Status AI.
Explore the Payor Denial Impact Report to understand how denial drivers, vague claim statuses, and rework affect reimbursement performance across diagnostic services—and where targeted AI can make the greatest impact.

