How Embedded AI Is Driving the Next Wave of RCM Innovation
Artificial Intelligence (AI) is increasingly being integrated into healthcare workflows, and its impact on revenue cycle management (RCM) is transformative. No longer a futuristic concept, AI already delivers measurable improvements in claim management, denial reduction, and financial outcomes. This article explores the impact of embedded AI in RCM for diagnostic organizations.
The Rise of AI in Revenue Cycle Management
AI is playing an increasingly vital role in optimizing RCM processes. The 2025 Payor Denial Impact Report reveals how native AI is enhancing the accuracy, speed, and efficiency of denial and appeal management:
- Predictive Analytics: For example, predicting which claims are more likely to be reimbursed, allowing staff to focus on high-value claims while avoiding investing valuable staff resources toward claims with a low likelihood of reimbursement.
- Deciphering Unstructured Text: For example, payor responses that require action, turning vague messages into specific steps for claim resolution.
Embedded AI: More Than Just a Tool
AI embedded directly into billing and reimbursement workflows offers distinct advantages. AI is only as powerful as the data it can access. Bolt-on solutions often struggle because they sit outside the core workflow and lack visibility into the full scope of financial and clinical information. By contrast, embedded AI operates directly within RCM systems, leveraging high-quality data in real time to automate tasks and deliver more accurate results.
Here’s how fully integrated AI is driving results:
- Faster Payment: AI speeds up the claim process by identifying and correcting errors before they lead to denials.
- Reduced Errors: AI helps ensure that claims are submitted with accurate patient and insurance information, reducing the time spent on rework.
- Increased Productivity: By automating routine tasks, AI allows staff to focus on higher-value activities, such as complex appeals.
Real-World Applications for Native AI in RCM
Embedded AI is already proving its value in multiple areas of the RCM process:
- Insurance Card Scanning: AI-powered tools can accurately capture insurance information, reducing errors in eligibility verification and improving the clean claim rate.
- Patient Responsibility Estimation: AI models predict patient out-of-pocket costs with greater accuracy, helping providers collect payments upfront and improve patient satisfaction.
- Prior Authorization: AI can help automate key parts of the prior authorization process, eliminating the need for manual intervention and reducing the time it takes to get approval for services.
Decoding Claim Status: Simplifying Interactions with Payors and Translating Payor Responses into Actionable Next Steps
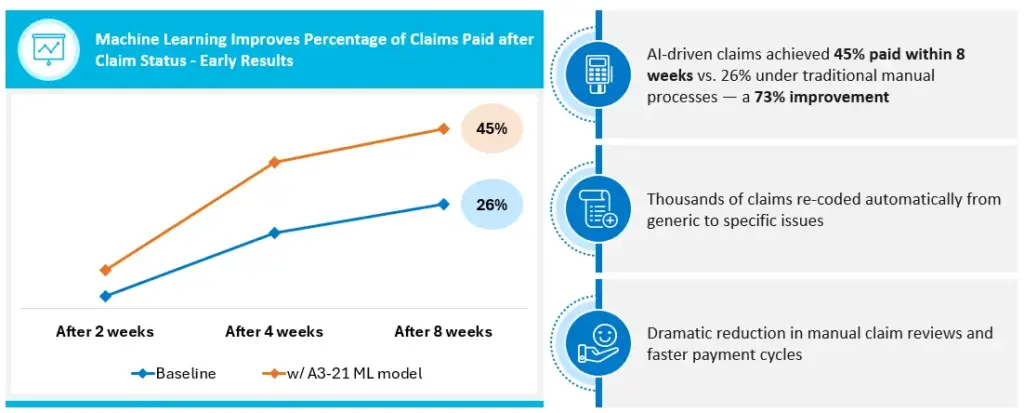
Among the most frustrating barriers to efficient claim resolution is the generic A3-21 status code, a catch-all indicator that something is wrong with a claim, but with no clear guidance on what needs to be fixed. XiFin addresses this by analyzing the associated free-text payor messages and translating them into specific, actionable categories such as “subscriber ID mismatch” or “invalid diagnosis code.”
This reduces the time staff spend deciphering vague messages and accelerates the resolution of issues. It also feeds into a real-time dashboard that allows managers to monitor trends, route work, and focus resources where needed most. Since its introduction, providers who have leveraged this capability have seen a 70% improvement in payment velocity compared to traditional manual processes within just eight weeks.
Measurable Impact Within 8 Weeks
AI-Driven Exception Processing: A Game Changer
One of the most powerful uses of AI in RCM is exception processing. AI-driven exception handling applies predictive models to prioritize claims based on their likelihood of reimbursement, ensuring that the most valuable claims are handled first.
- Faster Issue Resolution: Claims are triaged and routed to team members with historically the best success rates resolving particular error types, reducing the time it takes to fix errors by more than 40 percent, and improving productivity by close to 50 percent.
- Improved Payment Velocity: By predicting the likelihood of payment and routing claims to the most appropriate team members, errors are fixed faster, and reimbursements are accelerated.
The Future of RCM with AI
As AI continues to evolve, its impact on RCM will only grow. The 2025 Payor Denial Impact Report underscores that embedded AI is not a luxury; it is necessary for healthcare providers looking to stay competitive in an increasingly complex and competitive billing environment.
Embracing AI for a Smarter Future
AI-driven automation powers the future of RCM. AI is reshaping how providers manage their revenue cycle by automating routine tasks, enhancing decision-making, and improving claim accuracy. With smarter, faster workflows, fully integrated AI is not just improving operational efficiency; it is transforming the financial performance of diagnostic organizations, making it a crucial investment for the future.
